Recent POSTS
The blog post emphasizes the importance of intentional, curiosity-driven travel during a busy summer conference season, encouraging NIHD members to use professional gatherings as opportunities for meaningful connection, learning, and leadership in healthcare design.
It also offers practical travel and networking advice—such as packing strategically, allowing time for reflection, following up with new contacts, and observing how people interact with spaces—to inspire stronger collaboration and more human-centered design thinking.
This blog highlights the growing importance of advocacy in nursing, emphasizing how nurses translate real-world care experiences into policies and systems that improve healthcare delivery. It also underscores the expanding leadership role of nurses in innovation, technology, care design, and community impact, while encouraging nurses to actively shape the future of the profession through advocacy, collaboration, and lifelong learning.
The blog highlights the transformative impact of the $50 billion Rural Health Transformation Program, positioning it as a pivotal moment to redesign how care is delivered across rural America.
Rural healthcare design requires intentional, human-centered solutions that address scarcity, distance, and community needs while elevating clinical voices.
This investment is a rare opportunity to reshape not just facilities, but entire care systems and outcomes for underserved populations.
This blog profiles Sam Snell’s journey from a “wide-eyed and clueless” nurse to a leader in healthcare design and operations, highlighting how emergency departments reveal whether workflows and spaces truly function under pressure.
The blog highlights Angie Cox’s journey from social work to becoming a leader in clinical technology, driven by her belief that many healthcare challenges stem from system design rather than individual failure.
With multidisciplinary expertise, she works at the intersection of care delivery, technology, and strategy to create solutions that improve both patient and clinician experiences. Her work focuses on designing smarter systems that reduce burnout and make healthcare more effective and human-centered.
The future of healthcare design will not be defined solely by technology or efficiency, but by our ability to create environments that genuinely welcome.
At Stanford Medicine Children’s Health, smart sensor technology is transforming how healthcare spaces are used by replacing guesswork with real-time data. Thousands of sensors help staff quickly find and manage rooms, improving efficiency and the experience for patients and families while reducing unnecessary costs.
The approach also prioritizes transparency and privacy, ensuring data is anonymous and trusted. With plans to expand into air quality and energy monitoring, this innovation is shaping the future of smarter, healthier healthcare environments.
Emily Karbo, DNP, RN, EDAC, transitioned from a career in ICU nursing to healthcare design, using her clinical expertise to shape environments that improve patient care, staff workflow, and operational efficiency. Inspired by early experiences in hospice care and driven by a passion for human-centered design, she now blends compassion, collaboration, and innovation to make a lasting impact in the healthcare design community.
Nurses working in healthcare face growing clinical burdens, spending up to 40% of their shifts on indirect tasks like coordination and communication, contributing to burnout and turnover. Modern nurse call platforms such as Jeron’s Provider transform traditional call systems into intelligent workflow hubs by automating task routing, integrating with EHR and RTLS systems, and streamlining communication across departments.
By reducing non-clinical interruptions and improving response times, these systems free nurses to focus more on bedside care while improving operational efficiency and staff satisfaction.
This reflective post explores the NIHD member Jamie Hammer’s internal “GO or NO GO” debate about returning to school later in life to pursue a DNP after a long nursing career. Drawing on decades of experience—from bedside care to healthcare design—Jamie shares how professional maturity made advanced education more focused and manageable, and offers practical advice for choosing the right DNP program. Ultimately, earning her doctorate brought renewed purpose, a deeper appreciation for research and data, and a reminder that it’s never too late to keep growing!







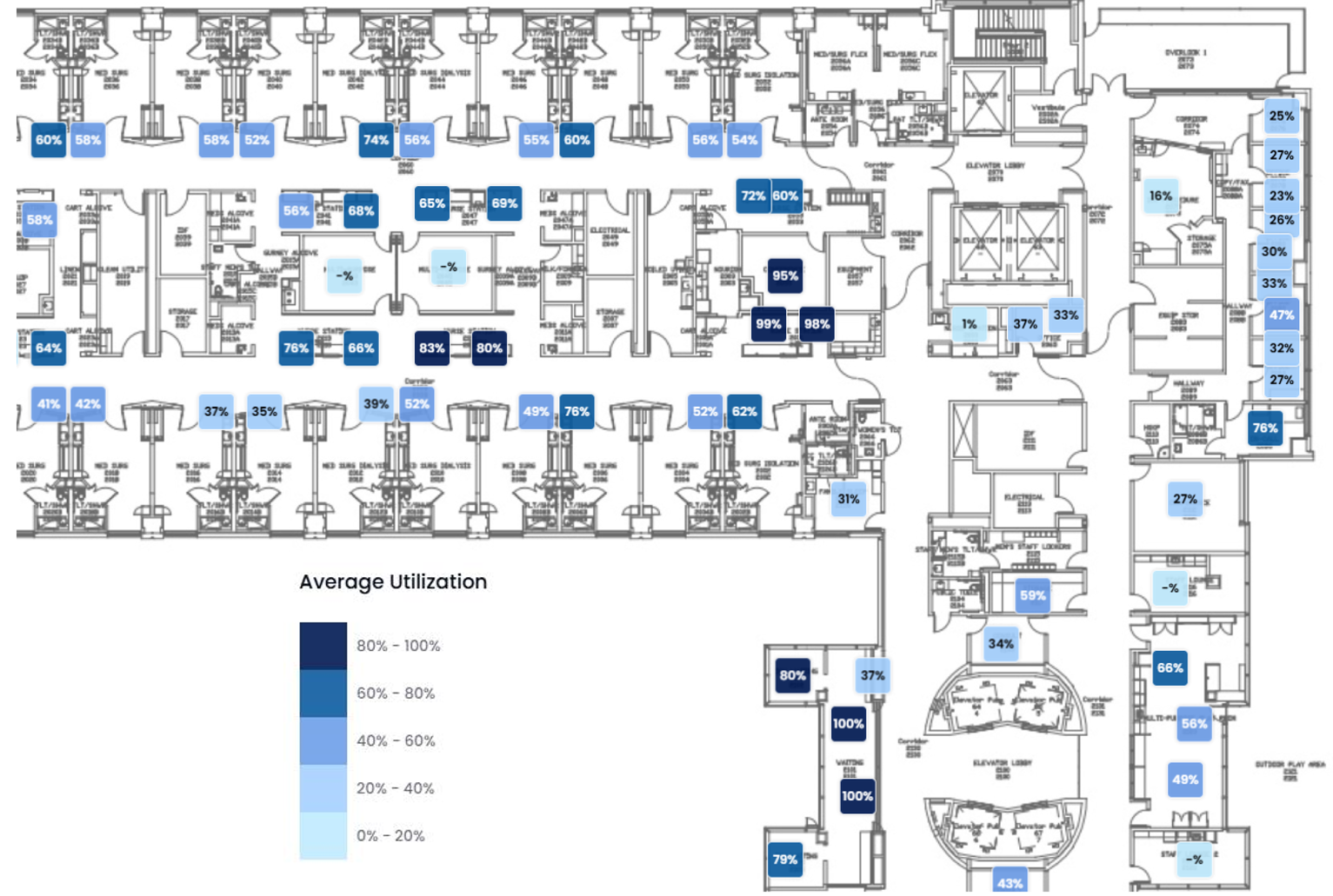



This blog features NIHD Board member Brooke Karlsen’s panel discussion at PDC Summit held in Houston in March 2026.
The intent of the session was to bring experts from across healthcare planning, design, engineering, and clinical communities to explore how resilient environments are created and sustained.
Through real-world examples and forward-looking strategies, the panelists were charged with providing insight into how healthcare spaces can remain safe, functional and supportive during times of crisis.